Claims Matrix FAQs
Visit Matrix > Claims for a comprehensive view of your claims.
Visit this report daily to e-File or print claims, address unpaid claims, and to find claims needing more information. Here are some commonly asked questions about the Tops Ortho Claims Matrix.
Why can't I see my Unpaid Claims?
- Don't worry; you still can! When you select the Unpaid Claims filter in the Claims Matrix, Tops Ortho defaults to showing you the claims in Rejected by Clearing House status. This is because these claims require your prompt attention.
- To see all of your Unpaid Claims, set the filters from left to right to:
- Unpaid Claims
- All Offices (or the office of your choice)
- All Submission Values
- Open Claims Only

What do the symbols in the second column mean?
These are indicators of claim type:
- A dot indicates an Initial Claim
- A diamond indicates a Pre-Estimate/Pre-Determination Claim
- No indicator present indicates a Periodic or Date-range Claim.

What do the yellow caution signs in the third column mean?
- The yellow caution sign will appear when the claim contains missing or incorrect information.
- Hover over the yellow caution sign to learn more about the missing/incorrect information.
- See related articles EClaims with Rejected by Clearing House Status and Common eClaim Rejection Reasons for more details.
Can I view this report by Insurance Company?
- Yes! Simply click the up/down arrow icon on the Employer heading and select Insurance instead.
-
Click the Insurance heading to group Insurers together.
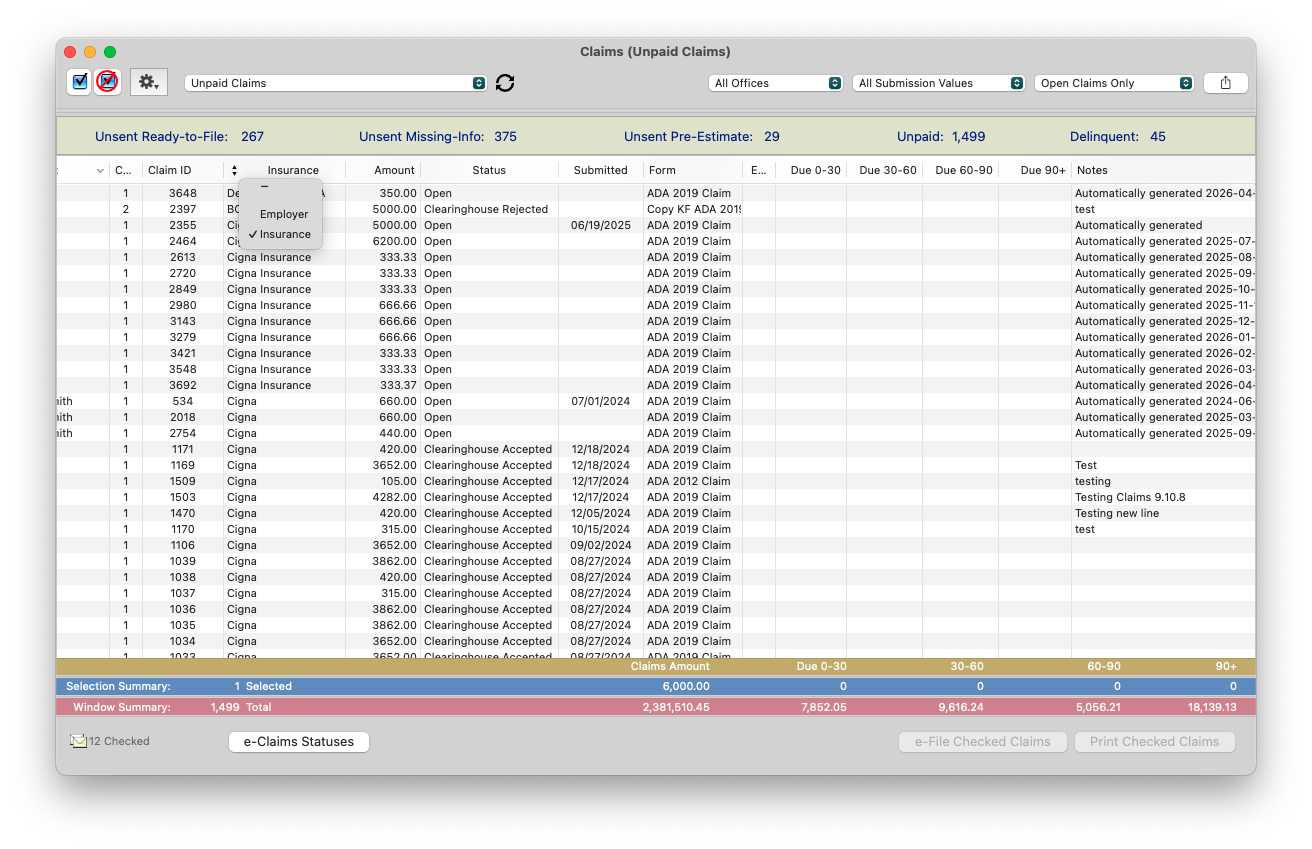
What information pulls in the Notes column?
- This column displays what is typed in the Internal Notes for this Claim field.
- To view or edit this field, right-click on the claim and select Edit Claim.

Why does my claim's aging reflect a question mark (?) ?
If a claim payment value reflects a question mark, it is due to the Employer Policy missing the payment percentage.


Why do I not see all my claims that are over 30 days old in the Delinquent Claims view?
Claims in the matrix are aged by generation date in the following ranges: 0 to 30, 30 to 60, 60 to 90, and Due 90+ (Due 90+ representing the final range of 90-120 days). Claims that remain open beyond 120 days will still appear in the Unpaid Claims Matrix under Open Claims Only, but will not display a possible payment value. Tops only represents values through 120 days.
Only open claims within the 0 to 120 day range that have an estimated payment value represented will appear in the Delinquent Claims filter.
My claim is more than 120 days old. Why is there not a value represented?
Tops will only show an estimated payment value with an open claim if the claim is between 0 and 120 days old. The age of the claim is based on the claim generate date, the first date represented in the claims matrix.
- Please read the section below titled Claims with Payment Values.
My claim is less than 120 days old. Why is there not a value represented?
- Date range claims do not display estimated payment values.
- The patient may not have a remaining benefit left to calculate a possible payment. Please read the section below titled Claims with Payment Values.

Should Expected Insurance match Claims Matrix totals?
The short answer is No.
Expected Insurance is calculated from ledger activity, making it a ledger-based value that is not directly tied to individual claims or the Claims Matrix.
The Claims Matrix, on the other hand, is claim-based and driven by employer policy calculations, remaining policy benefits, and existing open claims, rather than ledger balances.
Because these calculations are fundamentally different, the totals will not reconcile and are not intended to match.
Continue reading for a more in-depth understanding
Expected Insurance
Expected Insurance in the Accounts Receivable report represents the portion of a patient’s total balance that is anticipated to be paid by insurance. This amount is derived directly from the patient’s ledger and contributes to how the total balance is distributed across Due Now, Future Due, Copay, and Expected Insurance.
Expected Insurance is not a static value. It will fluctuate over time based on activity in the patient’s ledger. This includes the initial contract setup where a portion of the total fee is designated as expected insurance, payments posted from insurance carriers, and any manual adjustments made using Action and then Change Expected Insurance.
Because Expected Insurance is calculated from ledger activity, it is a ledger-based value and is not directly tied to individual claims or the Claims Matrix.
Claims Matrix
The The Claims Matrix reflects all open claims in Tops. Claims are generated based on qualified posted ledger activity, meaning transactions that have been designated to appear on a claim form, and how the claim is configured to generate based on the employer policy.
The Employer Policy determines when claims are created through settings such as claim frequency, claim type (manual or reminder), and payment calculation.
For example, if the claim frequency is set to Quarterly and the next claim date is 4/1/2026, Tops will review the patient’s ledger for any qualifying transactions posted within the previous quarter and generate a claim on 4/1/2026 representing those transactions and the amounts. These transactions may include automatically posted contract charges, such as scheduled monthly contract amounts, as well as manually posted transactions that have been marked to appear on a claim.
Claims with payment values
Initial claims and automatically generated claims include a possible payment value visible in the Claims Matrix under the 0-30, 30-60, 60-90 and 90+ columns. This value is calculated using the employer policy payment percentage and the patient’s remaining benefit on that specific policy. It is not based on the patient’s remaining Expected Insurance balance.
The system applies available benefits to claims by assigning possible payment amounts, starting with the oldest claim first. These values are reflected for claims within a 0 to 120 day aging period.
For example, if a patient has 400 dollars in their Remaining Benefit of the policy; a 50 % payment calculation represented in their employer policy; and five open claims for $200 dollars each, the system will apply the remaining benefit starting with the oldest dated claims. Each claim would have a possible payment value of $100. The first four claims will reserve the full $400 dollars of the patient's Remaining Benefit, and the fifth, most recent claim will display a $0 possible payment value since no benefit remains available. The Remaining Benefit is not the Expected Insurance. The Remaining Benefit is the remaining benefit the patient has with the policy.


